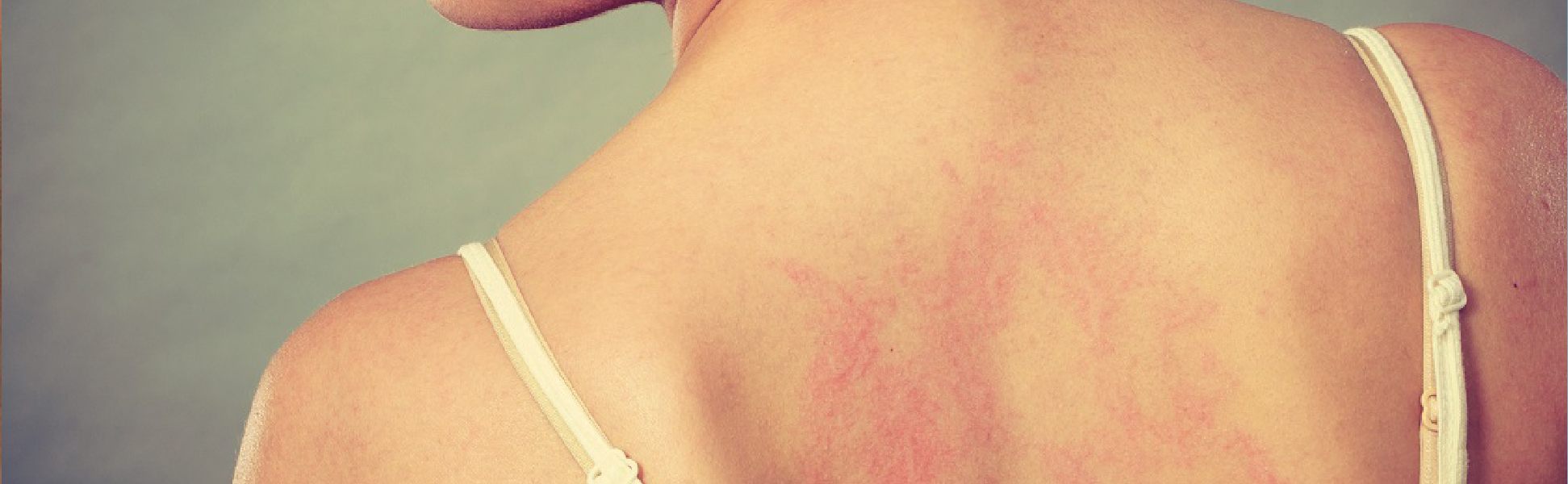
Atopic eczema is characterized by chronic, red, itchy rashes on the skin. It tends to spread, disappear and return on a regular basis. Simultaneously, it may lead to asthma and hay fever. This skin situation is mostly observed in children but can appear at any age.
It has affected 15-20% of children and 01-03% of adults worldwide.
Symptoms
Atopic eczema is first seen mostly in early childhood before the child is are 5 years old. Atopic eczema symptoms generally vary from person to person. Children may face the red, crusted, scaly areas on their cheeks, scalp, or the front of their arms and legs.
Additionally, it has been observed as very itchy, red rashes on the back of the neck, knees and in elbow creases for both children and adults. Few may have small bumps and flaky skin. Rashes on face, wrists, and forearms may also develop.
Other symptoms:
- Dry skin
- Itching, severe, especially at night
- Red to brownish-gray patches, especially on the hands, feet, ankles, wrists, neck, upper chest, eyelids, inside the bend of the elbows and knees, and in infants on the face and scalp
- Small, raised bumps, which may leak fluid and crust over when scratched
- Thickened, cracked, scaly skin
- Raw, sensitive, swollen skin from scratching
Diagnosis
No lab test is needed to identify atopic dermatitis (eczema). Physician/doctor will likely make a diagnosis by examining skin and reviewing medical history. Rarely, patch testing or other tests are performed to rule out other skin diseases or identify conditions that accompany your eczema.
Parents should informed about suspected food that cause rashes to their children to help find any food allergies.
Triggers
The factors that triggers or aggravate the atopic eczema are as below:
- Strong soaps and detergents
- Some fabrics, like wool or scratchy materials
- Perfumes, skin care products, and makeup
- Pollen and mold
- Animal dander
- Tobacco smoke
- Stress and anger
- Dry winter air/low humidity
- Long or hot showers/baths
- Dry skin
- Sweating
- Dust or sand
- Certain foods (usually eggs, dairy products, wheat, soy, and nuts)
Types
- Contact eczema: It is caused due to the direct contact of an irritant such as an acid, a cleaning agent, or other chemical
- Allergic contact eczema: The allergic reaction to the irritants in direct contact to the skin.
- Seborrheic eczema: It is a very common form of mild skin inflammation of unknown cause that presents as yellowish, oily, scaly patches of skin on the scalp, face, ears, and occasionally other parts of the body.
- Nummular eczema: It appears as round, isolated patches mostly on the arms and lower legs.
- Lichen simplex chronicus: It is caused due to long-term rubbing, scratching, or picking the any specific anatomic part of skin that is sensitive.
- Stasis dermatitis: It is irritation of the lower legs, generally due to circulatory problems and congestion of the leg veins. It may have a darker pigmentation, light-brown, or purplish-red discoloration from the congestion and back up of the blood in the leg veins. It is more common in legs with varicose veins.
-
Dyshidrotic eczema or pompholyx: irritation of the skin on the palms of hands (mostly) and less commonly soles of the feet. It is characterized by clear, very deep-seated blisters that itch and burn on palms and rarely on soles.
-
Xerotic eczema: It is characterized by areas of very dry skin most often seen on the lower legs of the elderly.
Treatment
As there is no cure for atopic eczema, treatment can only ease the symptoms. In children condition may naturally improve with time. The treatment does not usually require emergency therapy, but for treatment of acute flares caused by eczema herpeticum and bacterial infections.
- Emollients / moisturizers: They are used every day to relieve skin dryness.
- Topical corticosteroids: They are used to reduce swelling and redness during flare-ups.
Other treatments include topical pimecrolimus or tacrolimus for sensitive sites, antihistamines for severe itching, bandages or special body suits to allow the body to heal underneath, and targeted biologic therapy including Anti-IL-4Ra therapy (dupilumab), Anti-IL-33 therapy (ANB020), Janus kinase (JAK) inhibitors, and Topical phosphodiesterase-4 (PDE-4) inhibitors.